To get a better understanding of the equipment used in our glaucoma screening and diagnosis process, please read about the following diagnostic tests.
Glaucoma is referred to as the thief of sight and can be present without a patient even knowing. As the nerve fibers in the optic nerve are damaged in glaucoma, there is a gradual and painless loss of vision. Patients may not notice vision loss until they have more advanced stages of glaucoma. The term visual field refers to the area of a scene you can see with your eyes fixed on one location. For example, while watching a stop light, you may notice a car pulling up beside you in the next lane. Your peripheral vision enables you to see the movement of the car. The visual field is quite extensive when both eyes are working properly but with glaucoma, the field of view is reduced.
A visual field test measures two things:
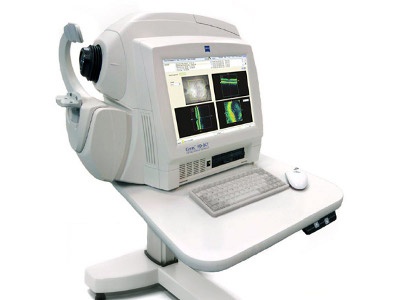
This device has the ability to capture images of eye tissue at a near individual cell level of resolution. In addition, it can show each layer of tissue in the eye allowing our glaucoma eye specialists to pinpoint the exact location of tissue damage. This sophisticated piece of equipment aids in the diagnosis and management of many ocular conditions, including glaucoma and macular degeneration. HD-OCT is a safe, painless and quick procedure that does not require dilation of the pupils. A laser scans the retina, optic nerve, cornea, or anterior chamber in just a manner of seconds to provide our glaucoma doctors with detailed information regarding the microscopic details of the eye. Anyone who has glaucoma or is a glaucoma suspect would benefit from undergoing this diagnostic test.
Pachymetry is the measurement of the thickness of the cornea, (the clear window on the front of the eye).
When the cornea is thinner than average, patients have an increased risk of developing glaucoma. When the cornea is thicker than average, patients have a reduced risk of developing glaucoma. Pachymetry should be performed at least once in a glaucoma patient’s adult life.
© 2025 Washington Eye Physicians & Surgeons
The material contained on this site is for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health care provider.